
Key Takeaways:
- ICHRAs are gaining momentum: Adoption is up 29% from 2023 to 2024, with a projected 255% increase by 2025.
- Technology is key to success: The right technology partner can streamline ICHRA administration and improve the employee experience.
- Education and awareness are crucial: Only 16% of respondents are fully confident in their understanding of ICHRA, indicating a need for more education.
- The insurance benefits field is embracing technology: 54% of respondents are using technology to support their business, with 19% identifying as innovators.
- Pending legislation could accelerate ICHRA adoption: The “One Big Beautiful Bill” Act could codify ICHRA as CHOICE arrangements and expand employer flexibility, potentially accelerating adoption.

AIM 2025 Premier ICHRA Conference, hosted by Remodel Health in Indianapolis, brought together technology vendors, brokers, health plans, and administrators gathered that all shared a similar purpose. Everyone believed in the potential of Individual Coverage Health Reimbursement Arrangements (ICHRAs) to bring flexibility and control to employers and employees alike, and the importance of finding a way to support ICHRAs success.
The conference provided a unique window into the challenges and opportunities shaping the future of health benefits. Kevin Deutsch, GM & SVP, and Tom Cohen, EVP, presented on the transformative power of technology in this space, and the importance of finding the right partner to navigate the complexities of ICHRA. Insights from a recent survey conducted by Softheon highlighted the real need for more benefit options, and the conference agenda reinforced the growing importance of technology in supporting ICHRA adoption and administration.
The Confirmed Need for ICHRA in 2025
A recent survey of 1,000 individuals conducted by Softheon revealed a landscape of concerns and opportunities that confirmed suspicions:
- Confidence gap: A staggering 86% of respondents lacked confidence in their plan selection, with 30% fearing they’d choose the wrong plan and 43% worried about limited provider choices. This uncertainty emphasizes the need for intuitive, user-friendly platforms that build confidence in employees to make informed decisions.
- Cost concerns dominate: A whopping 67% of respondents cited high costs as their primary concern, while 41% worried about coverage gaps. This highlights the imperative for cost-effective, personalized solutions that address the diverse needs of employees.
With these findings in mind, it’s no surprise that traditional group benefits are slowly decling in popularity.
- ICHRA adoption has surged 29% from 2023 to 2024, with projections indicating a 255% increase by the end of 2025.
- 83% of employers offering ICHRA or QSEHRA previously couldn’t offer insurance at all, demonstrating ICHRA’s potential to expand access to health benefits.
- Diverse Employer Uptake: Over 20% of small, 15% of mid-size, and 30% of large businesses are expected to offer ICHRA by year-end, underscoring the broad appeal of this innovative approach to health benefits.
Source: HRA Council; US Department of Labor
The appetite for more flexible, affordable health benefits is clear – and so are the real anxieties employees and employers face as they navigate this new landscape.
A Closer Look from the People There
W3LL’s breakout session focused on how to stay ahead of the curve with “Technology Transforming ICHRA.” The focus was put on the role of technology, finding the right partner that addresses the pain points we know exist, and making all the pieces work together harmoniously. As we delved into the challenges and opportunities of ICHRA, it became clear that there are specific pain points that need to be addressed in order to unlock the full potential of this health benefits.

A live survey was conducted during the session to gauge the audience’s perspectives on ICHRA and technology adoption. The results provided valuable insights into the ICHRA ecosystem:
- The make up of the room: The audience was comprised of a diverse group of stakeholders, including brokers/agents (13%), technology vendors (14%), health plans (11%), and others (23%).
- ICHRAs: A learning curve: When asked about their comfort level with ICHRA, 16% of respondents reported being fully confident, while 34% knew just enough but still had more to learn. 10% admitted they didn’t know where to start.

- Technology usage: A majority of respondents (54%) were already using technology to support their business, while 5% were not.
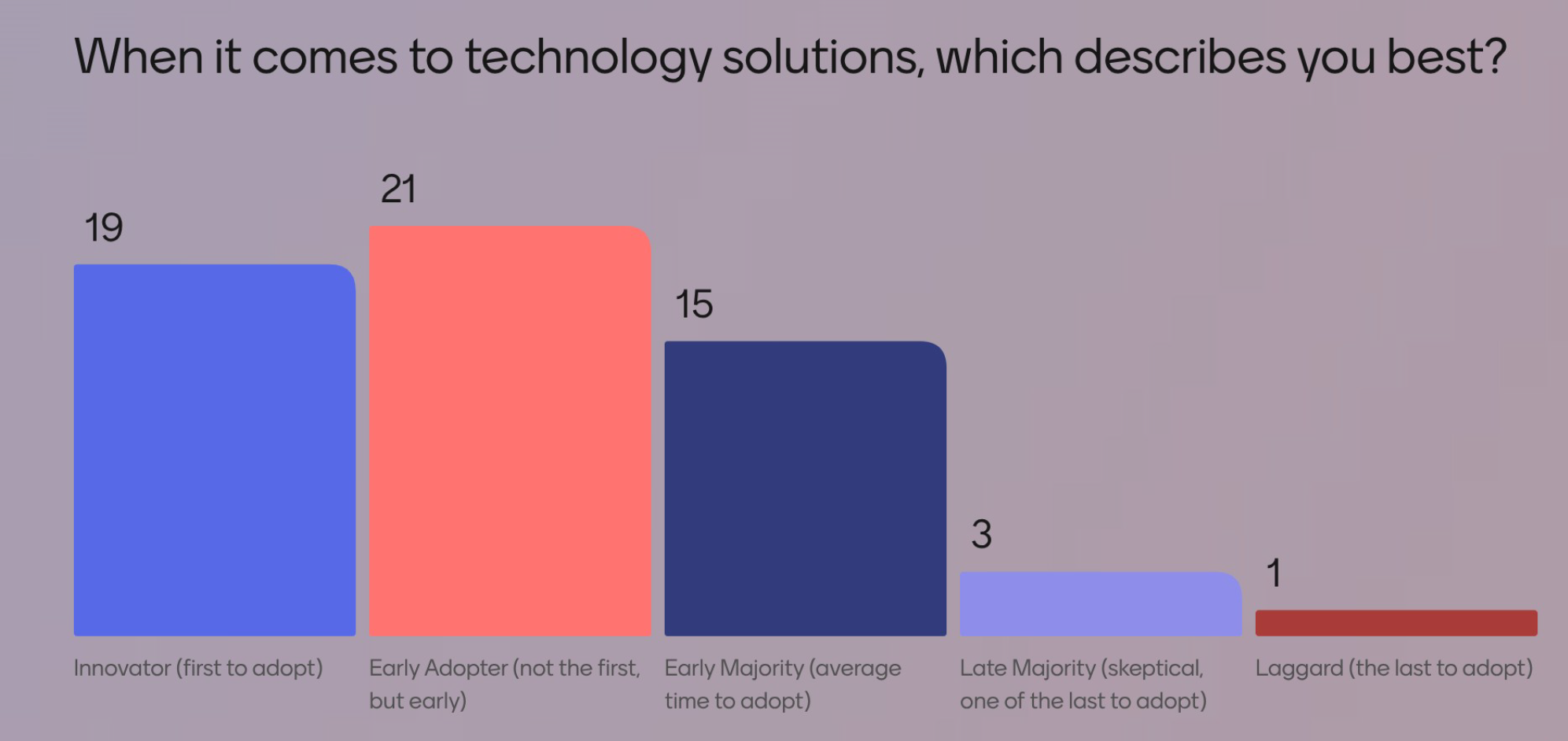
- Openness to innovation: When it comes to technology solutions, 19% of respondents identified as innovators (first to adopt), 21% as early adopters, and 15% as part of the early majority. Only 3% were skeptical and 1% were laggards.
- Reservations about adoption: While 42% of respondents had no reservations about adopting new ICHRA technology, 3% had concerns and 14% were still deciding.
- ICHRAs and technology: 36% of respondents were already using technology specifically for ICHRA business, while 16% were not. 7% wanted to but were unsure which solution to use.
- Confidence in ICHRA technology: Among those using ICHRA technology, 16% fully trusted it, 30% thought it worked but had room for improvement, and 5% didn’t trust it but had no other options.

These results also reinforced the opportunities available and where we need to continue putting our focus:
- ICHRAs are still a learning curve for many: The fact that under 50% of attendees felt confident in their understanding of ICHRA, suggests that there is still a significant need for education and awareness about ICHRA. This presents an opportunity for industry leaders to provide guidance and support to help stakeholders navigate the complexities of ICHRA.
- Technology adoption is on the rise: 54% of respondents were already using technology to support their business, and 19% identified as innovators (first to adopt). The industry is embracing technology as a key enabler of ICHRA’s success and this trend will likely continue. More organizations will be seeking out technology solutions to streamline ICHRA administration and improve the employee experience.
- Reservations about adoption are relatively low: Only 3% of respondents had reservations about new ICHRA technology, while 42% had no reservations. In fact, 36% of respondents were already using technology specifically for ICHRA business The industry is generally open to embracing new technologies and there is a growing recognition of the importance of technology in supporting ICHRA .
However, trust in ICHRA technology is a work in progress: Only 16% of respondents fully trusted their ICHRA technology, while 30% thought it worked but had room for improvement. This presents a huge opportunity for technology providers to focus on delivering high-quality, reliable solutions that meet the needs of stakeholders.
Overcoming ICHRA’s Growing Pains
As ICHRA adoption surges, the conference agenda and our presentation made it clear: Technology is no longer a nice-to-have, but a necessity for anyone looking to thrive in this space.
Key technology challenges include:
- Integration chaos due to inconsistent carrier connections across administrators
- Vendor overload, making it difficult to evaluate and select partners
- Data exchange disparities, with no standard file formats
- Operational inefficiencies in enrollment, billing, and payments
But don’t be too quick to pick a partner. Beyond just features, here’s what to look for in a technology partner:
- Seamless shopping and enrollment experiences for employees
- Streamlined payment processing and reporting
- Scalable solutions that support brokers, agents, and health plans as they grow
- Tools that help clients find better coverage and save money, while increasing engagement and lowering risk

The other conference sessions – ranging from “Winning with ICHRA” to “How Technology is Transforming ICHRA” and “The Rise of AI in Health Benefits” – all pointed to a single truth: Only with the right technology can organizations manage complexity, personalize benefits, and deliver exceptional experiences today’s employees expect.
The Policy Horizon: “One Big Beautiful Bill” and the Next Evolution
A recurring topic in both formal sessions and informal discussions was the pending “One Big Beautiful Bill Act.” This legislation, which passed the House, would codify ICHRA as the Custom Health Option and Individual Care Expense (CHOICE) Arrangement and further expand employer flexibility.
What’s Changing?
- Employers could offer both a group plan and ICHRA (rebranded as CHOICE Arrangement) to the same class of employees, letting workers choose the best fit.
- Notification periods for employees would be shortened from 90-days to 60-days, streamlining implementation.
- Pre-tax deductions for on-exchange premiums would be allowed, making ICHRA even more attractive.
If enacted, this bill will accelerate ICHRA adoption and push even more employers to seek out robust, integrated technology solutions. The ability to offer true choice and flexibility will only be meaningful if supported by platforms that make plan selection, enrollment, and ongoing administration simple and transparent.
Looking Ahead: Thriving in the ICHRA Era
The AIM 2025 conference confirmed that we are in the midst of a fundamental shift in how health benefits are delivered. ICHRA is not just a compliance solution – it’s a strategic lever for attracting and retaining talent, controlling costs, and empowering employees. But the path forward is complex, and the stakes are high.
As the ICHRA landscape matures, those who invest in the right technology – and the right partners – will be best positioned to thrive. The future of health benefits is here, and technology is the bridge to that future. With the potential passage of the “One Big Beautiful Bill,” the need to get it right has never been more urgent.
Looking for somewhere to start as you ramp up your technology? Contact W3LL today to learn more.


