Managing health insurance benefits has long been a complicated and time-consuming process. Employers face administrative burdens, employees struggle to navigate complex decisions with limited guidance, and brokers must manage renewals, ensure compliance, and stay ahead of a constantly evolving industry.
But change is here. Technology is reshaping how benefits are designed, delivered, and optimized and BenTechs are leading the charge. Their advancements are making benefits more user-friendly, personalized, and accessible, improving the entire experience for all:
- Employers benefit from administrative support solutions that simplify compliance and contributions
- Employees gain user-friendly shopping experiences that help them select the right plans with confidence
- Brokers can leverage modern tools to better serve clients and provide more flexible benefit options
This shift is redefining health insurance, and one of the most significant innovations is Individual Coverage Health Reimbursement Arrangements (ICHRA) — a flexible, tech-driven approach to benefits that provides employers, employees, and brokers with more choice and control.
ICHRA: A Game-Changer for Employers, Employees, Brokers, and BenTechs
As health insurance evolves, ICHRA has emerged as a flexible, cost-effective alternative to traditional group plans. Employees no longer want a one-size-fits-all benefits package. They expect customized options that align with their lifestyle, health needs, and financial goals. Employers can support this demand by adopting ICHRA, which gives employees full control of their healthcare journey.
Unlike traditional group health plans, ICHRA allows employers to set a defined monthly allowance for employees to use toward individual health insurance premiums and qualified medical expenses. This model shifts the power to employees, enabling them to select the plan that best fits their needs, rather than being forced into a limited selection of employer-sponsored options.
For ICHRA to function seamlessly, it requires the collaboration of brokers, BenTechs, and employers to drive adoption and create a smooth experience for employees. Each stakeholder plays a unique role in making ICHRA successful, from guiding plan selection to streamlining administration and enhancing accessibility. Here’s why ICHRA benefits all stakeholders:

With ICHRA at the center of this transformation, the shift toward personalized and proactive benefits selection is well underway — helping employers, employees, and brokers move beyond rigid group plans and embrace a smarter, more flexible approach to healthcare.
Personalized and Proactive Benefits Selection
ICHRA is driving one of the biggest transformations in the benefits space — giving employers greater cost control while empowering employees with more choices. When paired with technology-driven solutions, ICHRA reshapes how benefits are delivered, administered, and optimized.
Employers need administration support. ICHRA administrators like Enrichly and Savvi are simplifying the employer experience by providing tools that:
- Evaluate if ICHRA is the right fit for their business
- Establish employee classes to maximize benefits
- Manage contribution allocations for employees
Employees that are using their ICHRA funds to shop for an insurance plan are often using modern, user friendly platforms. BenTechs like Thatch and Gravie have revolutionized the insurance shopping experience, making it easier to:
- Filter and compare plans based on personal needs
- Understand costs and coverage options with greater transparency
- Feel confident in their plan selections. Based on a survey conducted by our parent company, Softheon, only 14% of respondents expressed confidence in their plan selection.
Brokers, who have traditionally helped employers navigate group plans, are evolving their role by guiding clients through ICHRA adoption. They now have access to technology-driven quoting and enrollment platforms that enable them to provide:
- Personalized recommendations for their employer clients
- Seamless integration with ICHRA administrators
- Ongoing support for employees navigating individual plan selection
Why ICHRA & Technology Go Hand-in-Hand
Technology isn’t just supporting ICHRA adoption — it’s making it viable at scale. New tech solutions ensure that ICHRA can be implemented efficiently while enhancing the experience for employers, employees, and brokers.
The success of ICHRA depends on technology-driven solutions that simplify plan selection, automate administration, and provide a seamless experience for all stakeholders. Here’s how BenTechs and other technology providers are making ICHRA work:
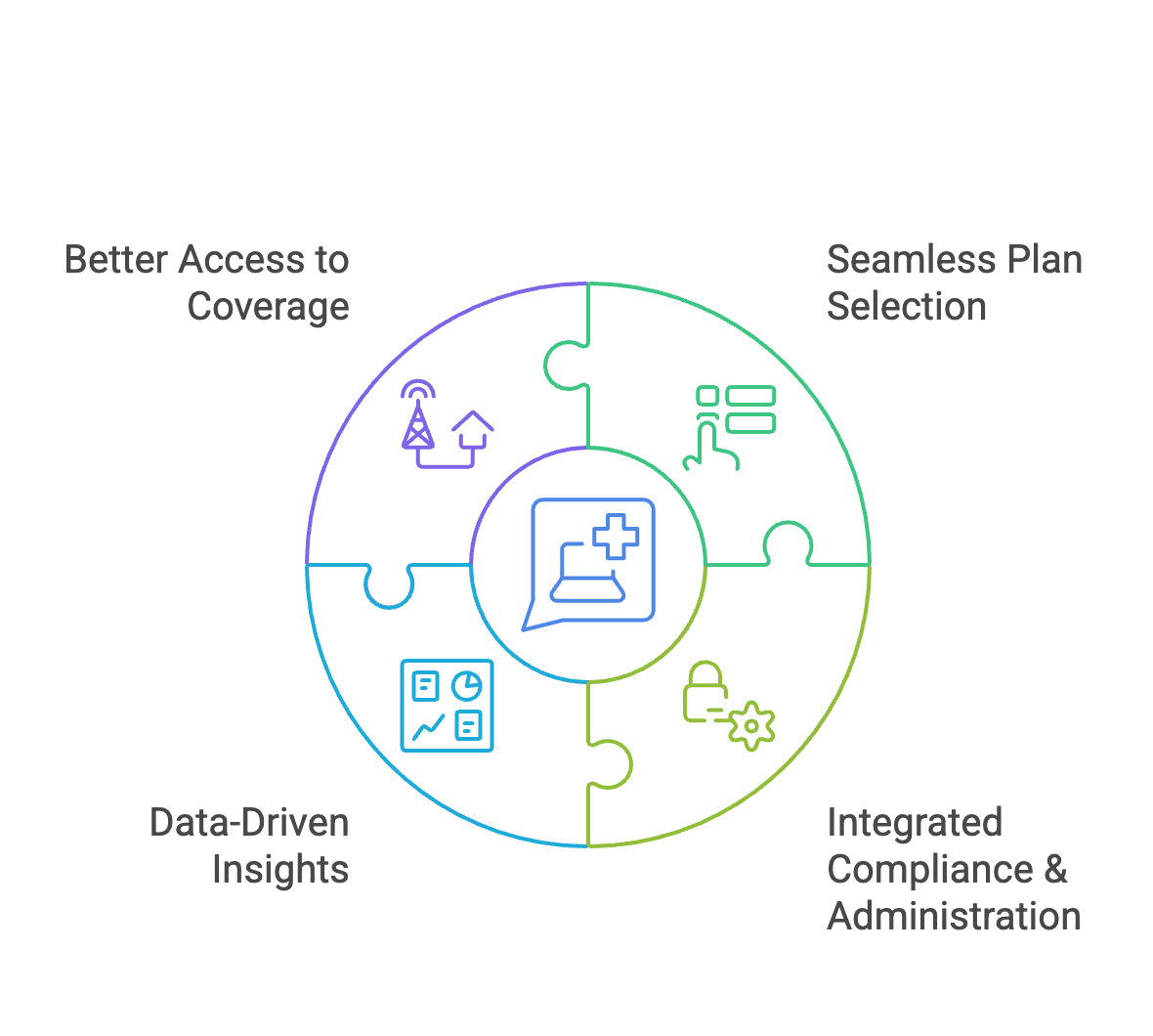
As more businesses move toward flexible, scalable health benefits, BenTechs and brokers are playing a key role in making ICHRA a reality.
Making Benefits More User-Friendly
The shift toward tech-driven benefits is well underway. According to Mercer Marsh Benefits, 50% of total HR budgets are being allocated to tech investments, marking a clear shift toward modernizing benefits administration. BenTechs, brokers, and technology-driven benefit partners are streamlining processes, improving accessibility, and delivering a more customized benefits experience.
Historically, selecting and enrolling in benefits has been a frustrating process. BenTechs are solving this pain point by introducing intuitive, digital-first shopping experiences. For employers, these innovations mean less administrative burden and more satisfied employees. For brokers, they provide smarter ways to support clients. And for employees, they deliver confidence that they’ve selected the best possible coverage.
The demand for personalized, flexible benefits has paved the way for ICHRA, and when paired with the right technology solutions, makes health insurance easier and more accessible than ever before.
The W3LL Advantage: Powering the Future of Benefits
While the benefits industry is evolving, one thing is clear: Technology is no longer a luxury. It’s a necessity. The need for modern, scalable solutions that enhance the employee experience, reduce administrative burdens for employers, and simplify benefits selection is crucial when empowering employees to make their own healthcare decisions.
At W3LL, we’re at the forefront of this transformation. We provide:
- Integrated technology solutions for BenTechs that simplify enrollment, improve accessibility, and streamline benefits administration
- Broker-focused platforms that automate workflows and enhance client management
- AI-driven insights to help brokers and employers make smarter, faster decisions
- Guidance for employees through clear, data-backed plan recommendations
The future of benefits is simpler, smarter, and more intuitive than ever before. BenTechs and brokers are leading this shift, and W3LL is here to help you embrace this transformation. Want to learn more about how W3LL can support you? Let’s talk.